GAS refers to a group of medical procedures that help align a person’s physical body with their gender identity. These surgeries are one part of gender-affirming care, which may also include social transition, hormones, voice therapy, and mental-health support. Not all transgender or nonbinary people want surgery, but for those who do, these procedures can significantly reduce gender dysphoria and improve quality of life.
Gender-affirming surgeries aim to:
Reduce gender dysphoria.
Improve psychological well-being and social functioning.
Help people feel more comfortable in their bodies.
Support congruence between physical characteristics, gender identity, and social attribution.
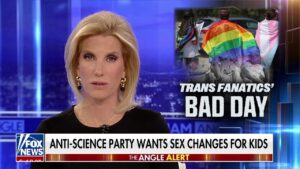
Use of the term “sex change” by Christian Nationalist-leaning media, and TERF/”gender critical” hate groups like Genspect and the American College of Pediatricians is an incendiary tactic, intended to trigger implicit and explicit bias.
Burleton Education is not a healthcare provider, and we do not, under any circumstances, offer medical advice. This content is provided for informational purposes only.
Always consult with a physician.
Neo-fascist, Christian Nationalism spreads disinformation claiming that minors (18 and under) are receiving (or being “subjected to”) “mutiliating” genital surgeries in the United States (and around the world).
Gender-Affirming Surgeries (GAS) have historically and currently very rarely been performed on anyone under 18 years of age, and never on pre-teen minors. As a result of intimidation of care providers, anti-trans legislation in many states, and pre-compliance by some risk-averse care providers and institutions, GAS on those under 19 years of age has been temporarily halted in many parts of the U.S.