Gender-Affirming Care:
Surgery
What is Gender Affirming Surgery? (GAS)
GAS refers to a group of medical procedures that help align a person’s physical body with their gender identity. These surgeries are one part of gender-affirming care, which may also include social transition, hormones, voice therapy, and mental-health support. Not all transgender or nonbinary people want surgery, but for those who do, these procedures can significantly reduce gender dysphoria and improve quality of life.
Purpose and Outcomes
Gender-affirming surgeries aim to:
Reduce gender dysphoria.
Improve psychological well-being and social functioning.
Help people feel more comfortable in their bodies.
Support congruence between physical characteristics, gender identity, and social attribution.
Medical Endorsements:
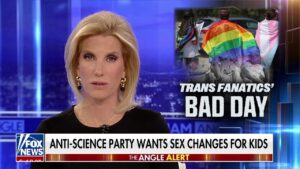
Use of the term “sex change” by Christian Nationalist-leaning media, and TERF/”gender critical” hate groups like Genspect and the American College of Pediatricians is an incendiary tactic, intended to trigger implicit and explicit bias.
Burleton Education is not a healthcare provider, and we do not, under any circumstances, offer medical advice. This content is provided for informational purposes only. Always consult a physician.
Burleton Education is not a healthcare provider, and we do not, under any circumstances, offer medical advice. This content is provided for informational purposes only.
Always consult with a physician.
MYTH
Neo-fascist, Christian Nationalism spreads disinformation claiming that minors (18 and under) are receiving (or being “subjected to”) “mutiliating” genital surgeries in the United States (and around the world).
FACT
Gender-Affirming Surgeries (GAS) have historically and currently very rarely been performed on anyone under 18 years of age, and never on pre-teen minors. As a result of intimidation of care providers, anti-trans legislation in many states, and pre-compliance by some risk-averse care providers and institutions, GAS on those under 19 years of age has been temporarily halted in many parts of the U.S.
Adolescent GAS
Description:
Removes breast tissue and reshapes the chest to create a flatter, more traditionally masculine contour.
Techniques include double-incision, periareolar, or keyhole, depending on chest size and skin elasticity.
Accessible for Trans+ Minors?
As a result of the current (2025) Christian Nationalist, authoritarian persecution of trans-spectrum youth, this is the one remaining gender-affirming surgical intervention that may be considered for some adolescents in rare cases, typically ages 15–17, when:
The young person has longstanding, well-documented gender dysphoria
They have been through a comprehensive evaluation with a mental-health provider experienced in gender care
They have parental/guardian consent
They demonstrate emotional maturity to understand risks and outcomes
Other steps (like social transition or hormone therapy) have already been in process
Even then, it is not routine and requires extensive assessment.
Description:
- Uses implants or fat grafting to increase breast size and achieve a more traditionally feminine chest appearance.
Accessible for Trans+ Minors?
As a result of the current (2025) Christian Nationalist, authoritarian persecution of trans-spectrum youth, this is the one remaining gender-affirming surgical intervention that may be considered for some adolescents in rare cases, typically ages 15–17, when:
The young person has longstanding, well-documented gender dysphoria
They have been through a comprehensive evaluation with a mental-health provider experienced in gender care
They have parental/guardian consent
They demonstrate emotional maturity to understand risks and outcomes
Other steps (like social transition or hormone therapy) have already been in process
Even then, it is not routine and requires extensive assessment.
These gender affirming surgeries are currently not available to those 18 and under in many places around the United States of America due to Christian Nationalist anti-science, anti-trans disinformation, and legislation.
Descriptions are provided for information purposes only.
Feminizing genital surgery (vaginoplasty and related procedures)
Creates a vagina, clitoris, and labia using existing genital tissue.
May also include orchiectomy (removal of testes) and vulvoplasty (creation of external genital structures without a vaginal canal).
Masculinizing genital surgery
Phalloplasty: Constructs a penis using tissue grafts (commonly from the forearm or thigh). Can include urethral lengthening, scrotoplasty, and placement of erectile or testicular implants at a later stage.
Metoidioplasty: Uses testosterone-enlarged clitoral tissue to create a smaller penis; may include urethral lengthening.
Hysterectomy/oophorectomy: Removal of uterus and ovaries for those who choose it.
Facial Feminization Surgery (FFS) and Facial Masculinization Surgery (FMS) are extremely rare for minors, and are not generally recommended or performed.
- For trans/nonbinary youth fortunate enough to have been on pubertal suppression treatment before Tanner Stage 3, and have had access to gender affirming hormone therapy, FFS and FMS may not be necessary, as their facial structure may not have been feminized or masculinized due to pubertal changes.
FFS/FMS are not recommended in major clinical guidelines, and most surgeons and hospitals will not offer it to anyone under 18.
Below is a clear explanation of why.
It involves major bony reconstruction (jaw, brow, chin, etc.).
Adolescents’ facial bones may not be fully developed.
Exceptions & Inequities:
Rhinoplasty ("nose jobs") procedures are commonly performed on cisgender minors for cosmetic purposes (as well as necessary medical reasons).
Rhinoplasty is usually delayed until the nose has finished most of its growth:
- Girls: typically 15–16 years old
- Boys: typically 16–17 years old
These ages vary because boys’ facial structures often mature later.
Short answer: In almost all cases, minors are not allowed to undergo feminizing voice surgery.
For trans girls who suppressed puberty before pubertal deepening of the voice, there is no need for feminizing voice surgery.
Here’s a clear breakdown of why and what the exceptions are:
Current Medical and Ethical Standards
Feminizing voice surgery (e.g., Wendler glottoplasty, cricothyroid approximation) is generally restricted to adults (18+).
Major professional organizations—including WPATH, the American Academy of Otolaryngology–Head and Neck Surgery, and most pediatric gender programs—consider voice surgery a procedure that should only be offered to adults because:
1. The larynx is still developing
Pubertal voice changes can continue into late adolescence.
Operating on a developing larynx can produce unpredictable or unstable long-term results.
2. Surgical risk and irreversibility
Voice surgeries permanently alter vocal fold structure.
Ethical standards require adult-level informed consent for irreversible changes.
3. Safer, effective alternatives exist for minors
Voice therapy with a licensed speech-language pathologist is considered the standard of care for minors.
Therapy can significantly feminize a voice without surgery.
Masculinizing voice changes usually occur with testosterone and are less likely to require surgery.
Liposuction or fat grafting to alter body shape is generally not performed on minors
Hair removal (electrolysis/laser) is allowed for minors, with parental approval.
Hair transplantation or scalp procedures for minors are generally not performed except in rare cases such as traumatic injuries, surgical scars, etc..
Take A Deeper Dive
Early 20th Century:
First "Modern" Surgeries (1900s–1930s)
Institute for Sexual Science (1919–1933)
Magnus Hirschfeld establishes the first institution dedicated to studying and advocating for the recognition and treatment of sexual and gender diversity. It is shut down, and all of its records (including those related to Karl Baer's surgical procedures) are destroyed (book burning) when the Nazis come to power.
Specialty Gender Clinics (1950s–1970s)
Europe
Georges Burou (Casablanca, Morocco; 1956–1970s):
Developed the pioneering penile inversion vaginoplasty, which remains the foundation of modern techniques.Christian Hamburger, Poul Fogh-Andersen, and others in Scandinavia refined feminizing surgeries.
United States
Academic programs began forming, often within university hospitals:
The Johns Hopkins Gender Identity Clinic (1966):
One of the first U.S. hospital-based programs offering evaluation and surgery.
Team included Dr. John Money, Howard W. Jones, Jr. (surgeon), and psychologist Richard Green.Stanford, University of Minnesota, Northwestern, and others opened similar clinics.
These programs:
Developed early surgical standards
Established psychiatric evaluation processes (the predecessors of WPATH SOC)
Trained surgeons in emerging techniques
However, due to political pressures and controversy, many U.S. clinics closed by the late 1970s.
20th Century: Expansion & Standardization (1980s–2000s)
WPATH and Standards of Care
The World Professional Association for Transgender Health (WPATH) (originally HBIGDA) created the Standards of Care (SOC) beginning in 1979.
SOC versions shaped clinical pathways for decades, standardizing:
Diagnostic criteria
Readiness assessments
Hormone therapy pathways
Surgical eligibility guidelines
Surgical advances
Refinements in penile inversion techniques.
Improved scrotoplasty and breast augmentation outcomes.
Development of minimally invasive metoidioplasty.
Expansion of facial feminization surgery:
Pioneered by Douglas Ousterhout (San Francisco) starting in the 1980s.
Globalization
Clinics expanded in Thailand (e.g., PAI, Bangkok Hospital, Yanhee), South America, and Europe.
Thailand became a major center due to its highly skilled surgeons and accessible regulations.
21st Century: Advancements, Recognition, and Diversity (2000s–Present)
Technical Innovations
Phalloplasty breakthroughs with radial-forearm, ALT, and other flaps.
Improved urethral construction and reduced complication rates.
Clitoral preservation and enhanced sexual function in vaginoplasty.
Robotic surgical approaches for hysterectomy and peritoneal vaginoplasty.
Widening adoption of robot-assisted peritoneal pull-through vaginoplasty since mid-2010s.
Institutional acceptance
Major medical bodies acknowledge gender-affirming surgery as medically necessary, including:
American Medical Association (AMA)
American College of Obstetricians and Gynecologists (ACOG)
Endocrine Society
American Psychiatric Association (APA)
Insurance and legal changes
Increased insurance coverage in the U.S., Canada, and Europe after the 2010s.
Broader legal recognition of transgender healthcare rights.
Nonbinary and individualized care
Surgical approaches have expanded to meet a spectrum of goals, not just binary affirming outcomes.
Current era
Gender-affirming surgery is now:
A globally recognized medical specialty
Based on evidence-driven outcomes
Integrated with interdisciplinary gender-affirming care
Continually improving in safety, precision, and patient satisfaction
For detailed, evidence-based clinical feminization info, visit UCSF.
General Risks of GAS
Every surgery carries some degree of risk. Complications vary by procedure and individual health factors.
Common Risks Across Most Surgeries
Bleeding
Infection
Poor wound healing
Scarring or keloids
Blood clots (rare but serious)
Pain, numbness, or altered sensation
Anesthesia risk
Procedure-Specific Risks
Chest Masculinization (Top Surgery)
Possible risks:
Nipple graft loss or reduced sensation
“Dog-ear” puckering at the sides of incisions
Hematoma (blood collection)
Asymmetry requiring revision
Hypertrophic scarring
Recovery overview:
Back to light activity: 1–2 weeks
Return to work (desk): 1–2 weeks
No heavy lifting: 4–6 weeks
Final chest shape: 3–6 months, sometimes longer
Scars fade over 6–18 months
Breast Feminization (Augmentation)
Risks:
Implant displacement or rupture
Capsular contracture (scar tissue squeezing the implant)
Need for future implant replacement
Nipple sensitivity changes
Seroma (fluid buildup)
Recovery:
Light activity: 1 week
Return to work: 1–2 weeks
Avoid chest exercise: 6 weeks
Final breast position (“drop and fluff”): 3–6 months
Vaginoplasty (Penile Inversion or Peritoneal)
Risks:
Vaginal stenosis (narrowing or shortening).
- Peritoneal vaginoplasty reduces this risk.
Loss or reduction of clitoral sensation.
Fistula (opening between the urinary tract/rectum, and vagina — rare).
Wound separation.
Granulation tissue.
Urinary issues (spraying, retention).
Hair growth inside the vagina if hair removal was incomplete.
- This risk is eliminated with peritoneal vaginoplasty.
Recovery:
Hospital stay: 3–6 days
Catheter: 7–10 days
Dilation schedule:
Weeks 1–12: several times daily
Months 3–6: daily
Months 6–12: a few times weekly
Walking normally: 4–6 weeks
Sexual activity: 3 months or when cleared
Full healing: 6–12 months
Phalloplasty
(One of the most complex gender-affirming surgeries)
Risks:
Urethral strictures (narrowing)
Urethral fistulas
Wound complications at the donor site (forearm or thigh)
Reduced sensation
Implant complications (if an erectile device is later added)
Higher risk of revision procedures
Recovery:
Hospital stay: 5–10 days
Catheter: 3–4 weeks
Donor-site healing: 1–2 months
Light activity: 3–6 weeks
Multiple stages are often required over 6–24 months
Sensation develops gradually over 1–2 years
Metoidioplasty
Risks:
Urethral strictures or fistulas (especially if the urethra is lengthened)
Dissatisfaction with size
Limited ability to stand-pee depending on technique
Recovery:
Catheter: 1–2 weeks
Light activity: 2–3 weeks
Full healing: 3–6 months
Facial Feminization / Masculinization Surgery (FFS/FMS)
Risks:
Nerve injury (temporary or permanent) affecting the forehead, lips, and chin
Hairline irregularity
Bone contour irregularities
Vision changes (rare)
Infection
Recovery:
Swelling, bruising: 2–6 weeks
Back to work (non-manual): 2–3 weeks
Final results: 6–12 months
Jaw, chin, and forehead procedures may take longer to settle fully
Voice Surgery (Pitch-Raising or Modifying)
Risks:
Hoarseness
Loss of vocal power
Difficulty projecting voice
Incomplete pitch change
Scar tissue on the vocal folds
Recovery:
Voice rest: 1–2 weeks
Resume speaking gradually over 6–8 weeks
Best results occur with post-op speech therapy
Emotional & Psychological Recovery
Important aspects of healing:
Hormonal fluctuations may affect mood.
Post-surgical emotional “dips” are common around weeks 1–3.
Social support and mental-health follow-up improve outcomes.
Many people report significant relief from gender dysphoria and improved quality of life after recovery.
Long-Term Outlook
Many people require one or more revision surgeries, especially with genital procedures.
Sensation often improves gradually over months to years.
Regular post-op checkups are essential.
A summary of the WPATH Standards of Care Version 8 (SOC8) guidelines related to eligibility for gender-affirming surgery. These are the current internationally recognized professional guidelines used by surgeons, insurance companies, and clinicians.
GENERAL ELIGIBILITY CRITERIA FOR ALL SURGERIES
These criteria apply across most procedures:
1. Persistent, well-documented gender incongruence/dysphoria
The individual has a consistent experience of gender incongruence.
This is documented by a qualified mental-health or medical professional.
2. Capacity to make a fully informed decision
The person can understand risks, benefits, alternatives, and expected outcomes.
3. Age considerations
SOC8 allows surgery for adults (18+) and adolescents under strict conditions.
For adolescents, additional requirements apply (multidisciplinary team, parental involvement, stable gender identity, etc.).
4. Any significant mental health concerns are reasonably well managed
Mental health problems do not disqualify someone; they simply must not impair the person’s ability to consent or follow postoperative care.
5. Physical health conditions are managed appropriately
E.g., diabetes, hypertension, nicotine use, bleeding disorders should be controlled for safe surgery.
6. Hormone therapy—not required for all surgeries
- SOC8 emphasizes that hormones are not mandatory for every surgery.
They are only recommended when hormones materially affect surgical outcomes.
HOW MANY READINESS LETTERS ARE REQUIRED?
SOC8 allows more flexibility than SOC7.
Typical expectations:
Chest surgeries: 1 letter
Genital surgeries: 1–2 letters depending on region, surgeon, and insurance
FFS/FMS: 1 letter
Voice surgery: 1 letter
Many surgeons now accept one comprehensive evaluation.
Adult GAS
Removes breast tissue and reshapes the chest to create a flatter, more traditionally masculine contour.
Techniques include double-incision, periareolar, or keyhole, depending on chest size and skin elasticity.
Uses implants or fat grafting to increase breast size and achieve a more traditionally feminine chest appearance.
Feminizing genital surgery (vaginoplasty and related procedures)
Creates a vagina, clitoris, and labia using existing genital tissue.
May also include orchiectomy (removal of testes) and vulvoplasty (creation of external genital structures without a vaginal canal).
Masculinizing genital surgery
Phalloplasty: Constructs a penis using tissue grafts (commonly from the forearm or thigh). Can include urethral lengthening, scrotoplasty, and placement of erectile or testicular implants at a later stage.
Metoidioplasty: Uses testosterone-enlarged clitoral tissue to create a smaller penis; may include urethral lengthening.
Hysterectomy/oophorectomy: Removal of uterus and ovaries for those who choose it.
Facial feminization surgery (FFS)
A collection of procedures that modify bone or soft tissue to create more traditionally feminine facial features (e.g., forehead contouring, jaw reduction, rhinoplasty).
Facial masculinization surgery (FMS)
Less common but may include chin augmentation, jaw implants, or brow augmentation.
Narrowing or tensioning of the vocal cords to raise pitch (for feminizing results).
Masculinizing voice changes usually occur with testosterone and are less likely to require surgery.
Liposuction or fat grafting to alter body shape.
Hair removal (electrolysis/laser) for feminizing results.
Hair transplantation or scalp procedures for masculinizing results.

